Introduction
Where family planning (FP) is concerned, women, men and young people who do not want to become pregnant but are not using contraception can utilize digital self-care platforms discreetly to expand their knowledge about family planning methods, counter misconceptions, and access services. Thus, such platforms can contribute to shifting two key behavioral outcomes: increasing uptake of family planning and ensuring correct and consistent use of contraceptive methods.
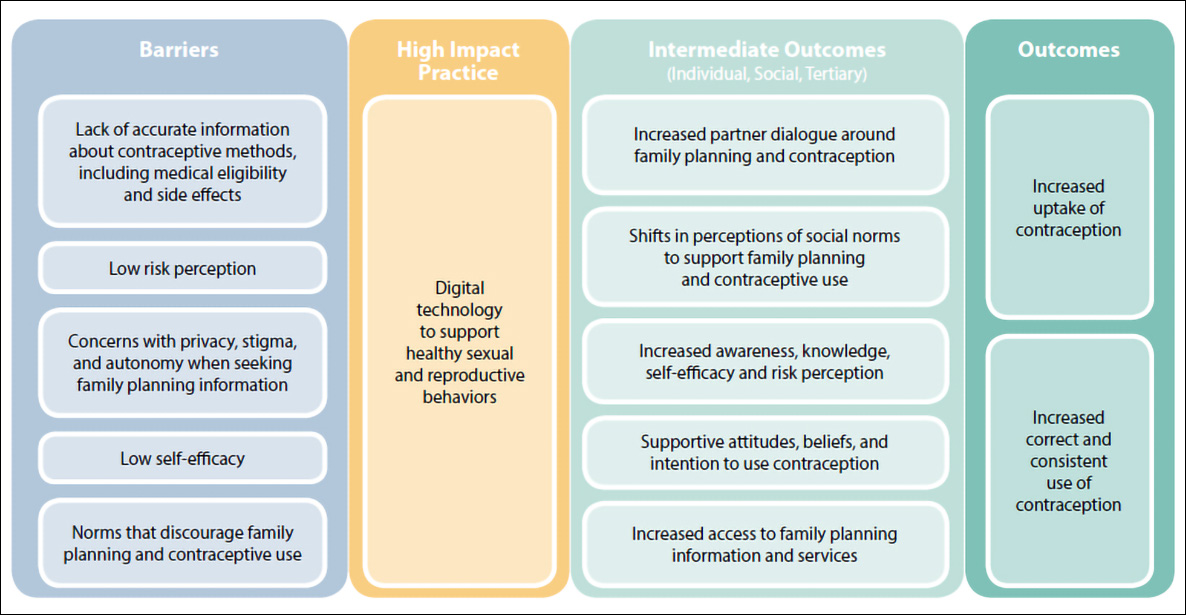
Figure 1: Theory of change published in the Digital Health for Social and Behavior Change High Impact Practice Brief
In this blog post, I describe the state of the evidence base for social and behavior change digital interventions that aim to support users in family planning, detail challenges related to research design that have led to these evidence gaps and share findings from four different studies that represent distinct LMIC-based implementation experiences of the theory of change (Figure 1).
The evidence and the challenges
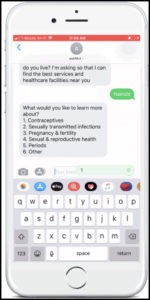
Image from m4RH, FHI 360’s SMS-based digital self-care
However, evidence about whether digital self-care tools increase adoption of FP methods and continuation remains limited, partly because of the following reasons:
- Digital health is often part of a constellation of interventions, so it can be difficult to isolate its effects. As a result, there are few gold standard randomized control trials (RCT) studies for digital SBC interventions.
- Often, study participants are recruited virtually, which can therefore lead to greater attrition.
- Engagement with digital platforms is variable, which makes it difficult to meaningfully understand efficacy.
- The technology used in digital health tools is rapidly evolving, so it is difficult for the evidence to keep up.
In our endeavor to explore the questions above, my colleagues from the Research for Scalable Solutions project (R4S) and I set out to contribute to the digital self-care knowledge base in three concrete ways by:
- Improving the quality and design of digital FP self-care interventions
- Producing evidence about what works and why to inform implementation and scale
- Building consensus around methods and measures for research on digital FP self-care
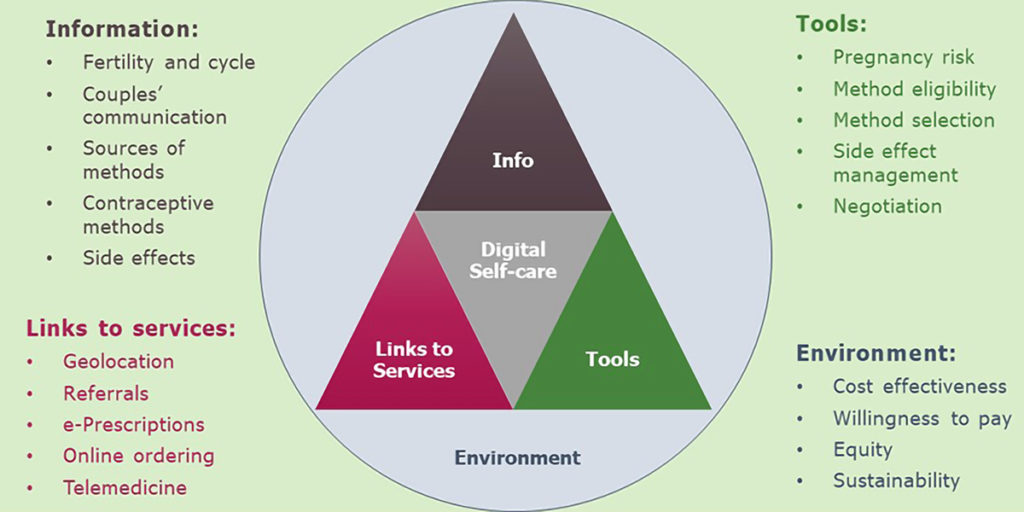
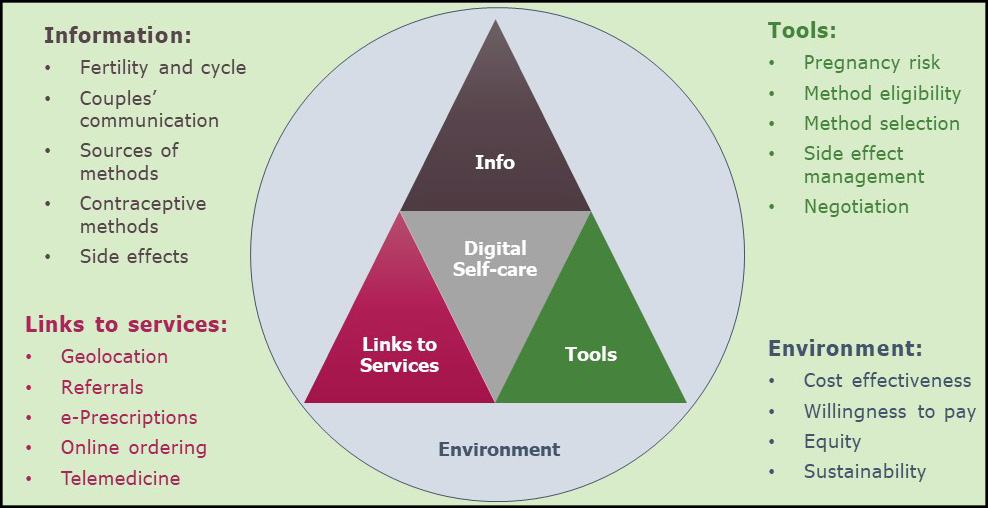
To do so, we first considered digital self-care tools based on how they aim to serve users – by providing general information, tailored information, tools or assessments, or links to services (Figure 2).
We then developed a set of research questions with attention to specific emerging themes:
- Acceptability and feasibility: How do users feel about interacting with the platforms?
- User experience: How do users interact with the platforms?
- Outcomes measurement: Do the platforms work?
- Cost: How much do the platforms cost?
Bearing our framework in mind and to expand evidence on digital platforms making use of newer technologies in real-world conditions, we decided to partner with askNivi in India, Ylabs’ CyberRwanda in Rwanda and PSI’s Counseling for Choice in Cote d’Ivoire, ensuring we address the research questions from multiple vantage points.
askNivi
The AskNivi chatbot provides sexual and reproductive health information, screenings and referrals to products and services in the public and private sectors to users across Kenya, Nigeria, South Africa and India. By increasing knowledge about fertility, contraceptive methods and where one can obtain them, askNivi can increase uptake and ultimately, continuation since askNivi also provides tailored follow-up support.
CyberRwanda
By providing digital access to reproductive health and FP information through storytelling and direct links to local youth-friendly services, CyberRwanda has three primary objectives: to increase FP uptake, delay initiation of childbearing, and increase rates of HIV testing among Rwandan adolescents ages 12-19.
Our study is focused on youth center implementation, complementing a separate RCT of the school-based model. We use a serial cross-sectional design to assess the intervention’s effects on relevant behavioral outcomes, including intent to use a modern method, perceived norms and knowledge related to fertility awareness and contraceptive methods. The study will also generate evidence about the potential for financial sustainability from CyberRwanda user, implementer and stakeholder perspectives. Ultimately, the generation of multi-faceted evidence can guide decisions about future implementation and scale-up.
Counseling for Choice

Gabi, modeled after an Ivorian nurse, offers a personalized experience based on user’s responses to a set of questions.
Counseling for Choice leverages choice architecture to provide information in an easier-to-understand format focusing on user’s priorities and preferences, implemented by PSI in Benin, Malawi, and Cote d’Ivoire. Originally developed as a training and counseling approach for FP providers, Counseling for Choice is a client-facing tool that engages users in a conversation about their preferences and FP needs through a chatbot. It aims to increase knowledge and service utilization, ultimately leading to increased method satisfaction and continuation.
Who will interact with the chatbot? How will they find it? What will they think and do? Our study of this intervention uses a descriptive, mixed methods design using surveys, back-end data and qualitative interviews to explore the user population based in Côte d’Ivoire and their experiences.
Looking ahead
We look forward to learning from the findings from these studies and to the opportunity to explore replication or expanded implementation of these and other digital self-care interventions. Each study will be broadly disseminated in the countries in which they were conducted and globally to help promote greater uptake of the results and to advance thinking on appropriate methods and measures for research on digital platforms.
We know there are others who are working diligently to advance the evidence in digital self-care. To support our digital health community to be better informed, coordinated and aligned, we hope to convene those currently conducting research on digital self-care for FP in 2023 to document what evidence is coming down the pipeline, determine what gaps remain so as to help direct future research, and share best practices relating to research design and methods.
Interested? Please email us to be added to R4S’ digital portfolio distribution list.
Photo Credit: FHI 360