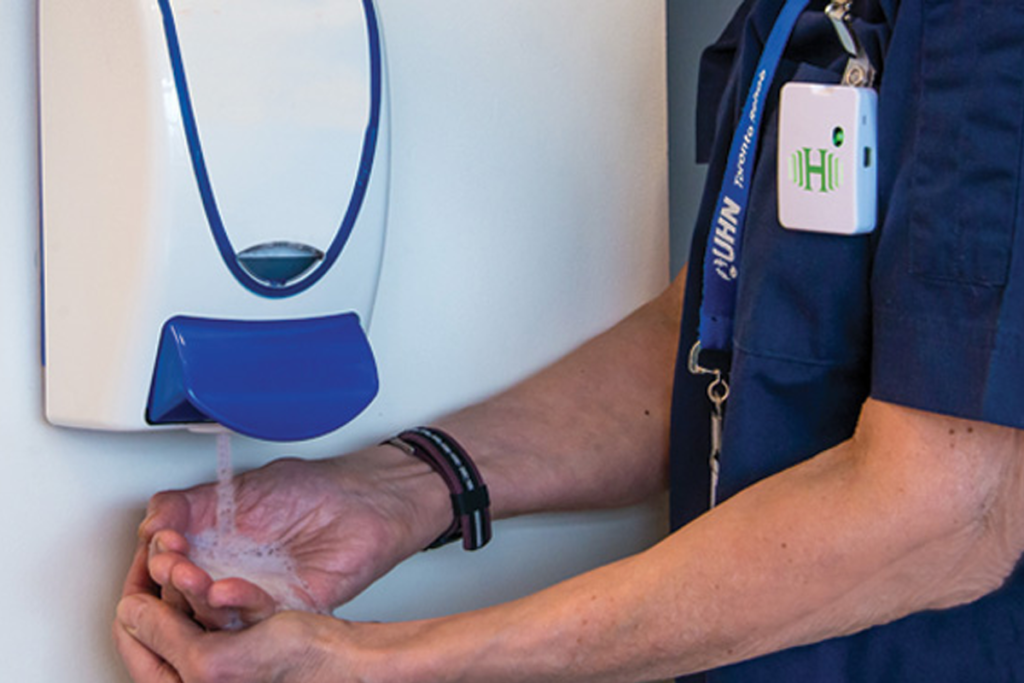
I recently read a post highlighting an innovative and evidence-based solution to a consistently overlooked (but important) issue – hand hygiene in health care settings. Maureen Banks shared how the use of sensing technology improved hand hygiene compliance and reduced C. Difficile infection rates by 75% at her post-acute care hospital. In facilities like Banks’ hospital, where patients experience a longer average length of stay, proper hygiene infrastructure and practices are especially important in reducing infections.
The World Health Organization (WHO)’s guidelines on hand hygiene push for new innovations and technologies to be developed to better measure hand hygiene practices. As highlighted by Banks, sensing technology is an emerging evidence-based strategy to measure and promote hand hygiene. In this post, I focus on evidence showing sensing technology as a reliable (perhaps superior) method for measuring and guaranteeing hand hygiene compliance.
What is hygiene-specific sensing technology?
Hygiene-specific sensing technology is designed to ensure health care workers perform hand hygiene during WHO’s Five Moments for Hand Hygiene (critical moments of care). It increases accountability, provides a monitoring system, and creates an overall sense of ownership among health care workers.
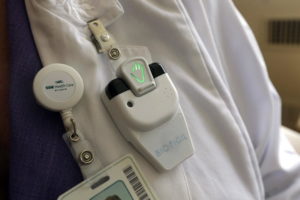
The technology records and promotes hand hygiene compliance (Marra and Edmond, 2014) using a special badge (a variation pictured at right) with colored lights to indicate hand hygiene status – green means hand hygiene has been performed, yellow is a reminder to clean hands, and red means hand hygiene should occur immediately.
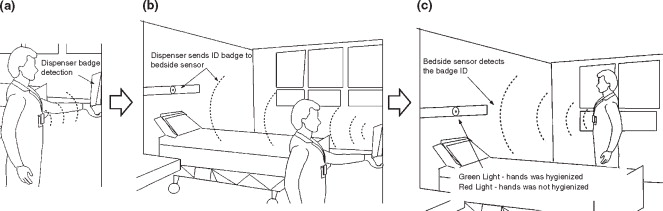
The image below provides an illustration of how that works. A sensor in the badge automatically communicates with transmitters at key points in a patient’s room (e.g., the room entrance/exit and patient bedside), detecting when there is a hand hygiene opportunity.
Health care workers have up to 60 seconds to confirm that their hands have been cleaned with alcohol-based handrub by cupping their hand over the badge. Sensors in the badge detect alcohol vapors and determine whether there is enough alcohol on their hands to indicate good hand hygiene. If yes, the light turns green. If no (or if the worker doesn’t cup their hands over the badge at all – i.e., didn’t clean their hands), the badge displays a yellow or red light to indicate a missed hand hygiene opportunity. This yellow or red light notifies patients and other health care workers of the worker’s hand hygiene status. Often, depending on the variation in the sensing technology format, this visual nudge may also be accompanied by a vibration or an audible ping nudge as well.
Monitoring and guaranteeing hand hygiene compliance with sensing technology
Sensing technology has been proven to increase hand hygiene compliance rates. A study by Edmond et al. (2010) [gated] used four weeks of direct observation (the gold standard of hand hygiene measurement), followed by a two-week evaluation of a sensor technology system to assess the impact of sensing technology for monitoring hand hygiene compliance.
In the first study phase, Edmond et al. observed 1,646 hand hygiene opportunities through direct observation with a compliance rate of 66%. In the second phase, the researchers electronically monitored 6,831 opportunities using sensing technology with an overall compliance rate of 93%. Segmented regression analysis showed a 23% increase in measured hand hygiene compliance immediately following the implementation of sensing technology. The captured data on hand hygiene moments improved the ability of health care staff and their supervisors to recognize current gaps in hand hygiene, holding health care workers more accountable to clean their hands during critical moments of care. This study, like many others, found that the use of sensing technology for hand hygiene monitoring can result in improved compliance rates.
Direct observation has long been considered the gold standard for measuring hand hygiene compliance because it provides the most information. However, it tends to be labor intensive and costly. Direct observation also has limitations with validity, including reliability, sampling bias, and concerns regarding patient privacy. Sensing technology, on the other hand (pun intended), may be a superior alternative to direct observation that addresses these limitations.
For example, Grenado-Villar et al. (2011) explored the technology’s reliability in tracking the number of hand hygiene opportunities during critical moments of care. In their presentation at the 2011 Society of Healthcare Epidemiology of America Meeting, Grenado-Vilar et al. reported 100% accuracy of the sensing technology system during their study period. In the study, the researchers examined a monitoring system, which included a bed monitor, electronic badge, and handwashing station that recorded hand hygiene opportunities. They found correlations between the use of sensing technology and hand hygiene behavior.
According to Grenado-Villar et al.’s findings, the use of sensing technology (compared to direct observation) is a more comprehensive way to measure the proportion of hand hygiene opportunities taken. While there are some limitations to sensing technology, such as lack of context-specific data (Boyce, 2015), sensing technology can provide real-time analysis and feedback on hand hygiene activities.
Further research on sensing technology is still needed. Most studies are limited to short study periods and some have failed to establish the badge’s sensitivity (e.g., measures truly clean hands) and specificity (e.g., measures truly unclean hands) of compliance rates, which is an important measure of accuracy. Nonetheless, the most interesting aspect of sensing technology for me is its ability to motivate health care workers’ decisions. The use of visual nudges (colored lights) on badges provides an accountability mechanism among peers and patients and provides a personal reminder to health care workers to clean their hands. Rather than a generalized handwashing sign, sensing technology is individualized to the health care worker, providing a color-coded image of their own actions.
What does this mean?
With an end goal of improving patient outcomes, the evidence around sensing technology points to an innovative way to measure and improve hand hygiene practice among health care staff. Ultimately, the power of accurate and centralized data paired with the immediate reminders from their badges keeps health care workers more accountable for their hand hygiene practices, allowing them to better connect their own hand hygiene behaviors with their role in preventing infections and providing safe care.
Photo credit: Barry Westhead/TRI